 Suicide is a national public health issue among the general population, and especially for those who have served in the military(1). Research in military, Veteran and civilian populations has shown that one of the highest periods of risk immediately follows discharge from psychiatric inpatient treatment and the highest numbers of death by suicide were reported in the days immediately following discharge(2,3). To address this this high risk period, Dr. Bridget Matarazzo, PsyD, of the Department of Veteran Affairs Rocky Mountain Mental Illness Research Education and Clinical Center (MIRECC) and the University of Colorado and her colleagues developed the Home-Based Mental Health Evaluation (HOME) Program to better engage patients in care after hospitalization(4).
Suicide is a national public health issue among the general population, and especially for those who have served in the military(1). Research in military, Veteran and civilian populations has shown that one of the highest periods of risk immediately follows discharge from psychiatric inpatient treatment and the highest numbers of death by suicide were reported in the days immediately following discharge(2,3). To address this this high risk period, Dr. Bridget Matarazzo, PsyD, of the Department of Veteran Affairs Rocky Mountain Mental Illness Research Education and Clinical Center (MIRECC) and the University of Colorado and her colleagues developed the Home-Based Mental Health Evaluation (HOME) Program to better engage patients in care after hospitalization(4).
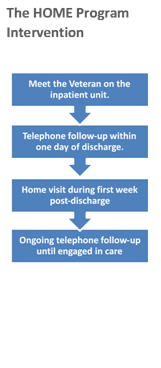
The HOME Program consists of four main parts: (1) meeting with the Veteran on the inpatient unit to introduce the program and schedule follow up appointments, (2) completing a telephone follow-up within one day of discharge, (3) performing a home visit within the first week of post-discharge, and (4) conducting ongoing telehealth follow-up – at weekly intervals – until the Veteran is engaged in care. During these contacts, the HOME Program provider assesses risk, reviews and updates the Safety Plan, and identifies and problem-solves around barriers to care.
Following a small study with promising findings4, Matarazzo and colleagues conducted a multisite, two-arm trial that compared the HOME Program and enhanced care as usual (E-CARE) at four participating psychiatric inpatient units5. A final sample of 302 (166 HOME Program and 136 E-CARE) participants were enrolled in the study. Veterans enrolled in the HOME Program were significantly more likely to engage in outpatient mental health care after discharge and attended more individual mental health sessions as well as engaged more quickly than those receiving E-CARE. Request for additional information about the HOME Program can be sent to the VA Suicide Risk Management Consultation Program at srmconsult@va.gov to set up a free consultation to discuss next steps.
References